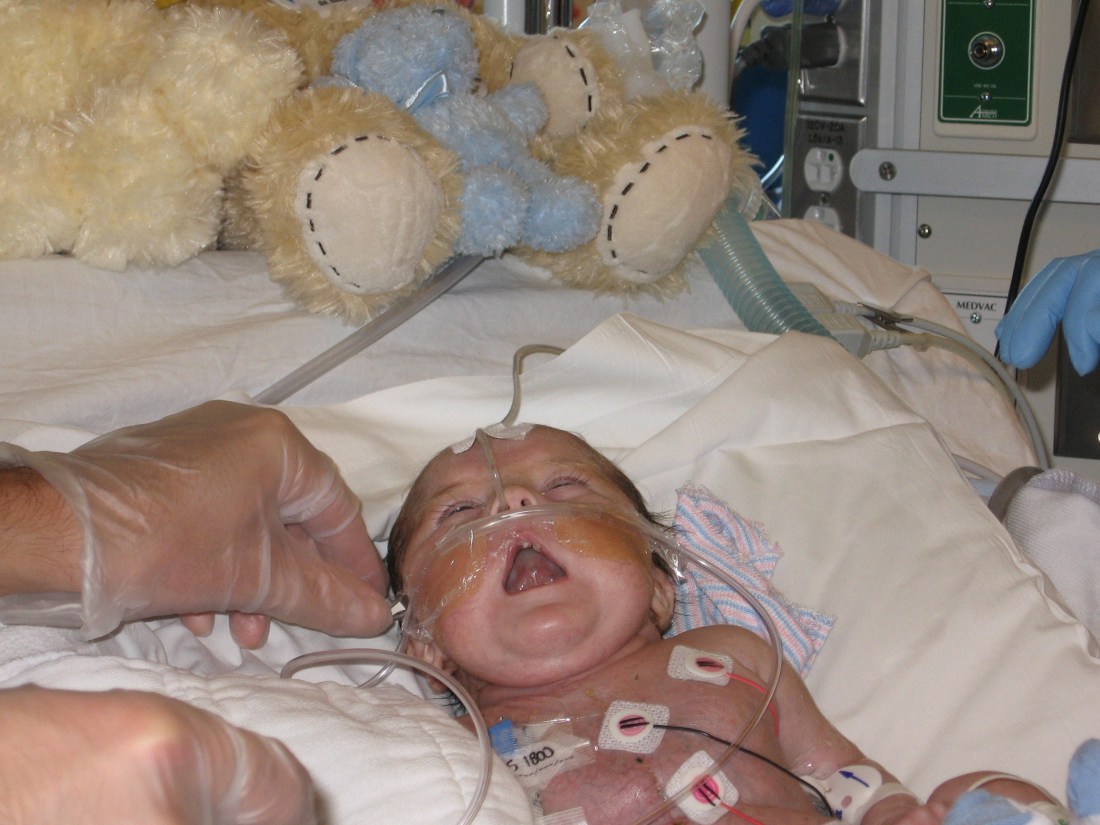
We were so excited to see the wait for a donor heart come to an end last week for Cesar. As he battles back after his transplant in the room next door, having learned the hard way that In-N-Out and Burger King might not be the best in post-op nutrition, here’s more of his story:
There’s a regular shuffling of the chairs between rooms here in the CTICU. If we find ourselves short, I check through vacant rooms to see what I can find. The nurses tend to be concerned for our comfort and often lead the search for a nice rocker or recliner if we look like we need it. While our stay is approaching a length to where we feel enough ownership over this room that we might repaint it, there’s no dibs on the furniture and if the nurses need it, they have no problem coming for it.
I remember coming in one morning the week before Halloween to find that all of our chairs had been cleaned out. As I set off on my quest, a nurse explained that several family members of the newly arrived patient next door had spent the night and needed lots of chairs.
Introductions between neighbors in the ICU tend to be slow in coming. Most families come in shocked and are so focused on what’s going on with their child that there really isn’t much attention left to be paid to meeting the neighbors. Many kids are only in the unit for 2-3 days until they’re stable enough to be moved to the floor, so it usually takes seeing the same faces for about five days before one gets introduced and acquainted.
For about that long, I noticed a steady stream of people coming and going from the room next door. Walking by, I caught glimpses of the tall kid laid out on the bed with the usual tubes and hoses. Like most patients, he came in here in pretty rough shape but after a few days I noticed his eyes would be open and he’d be holding court with nurses, doctors or the guests that always seemed to be visiting.
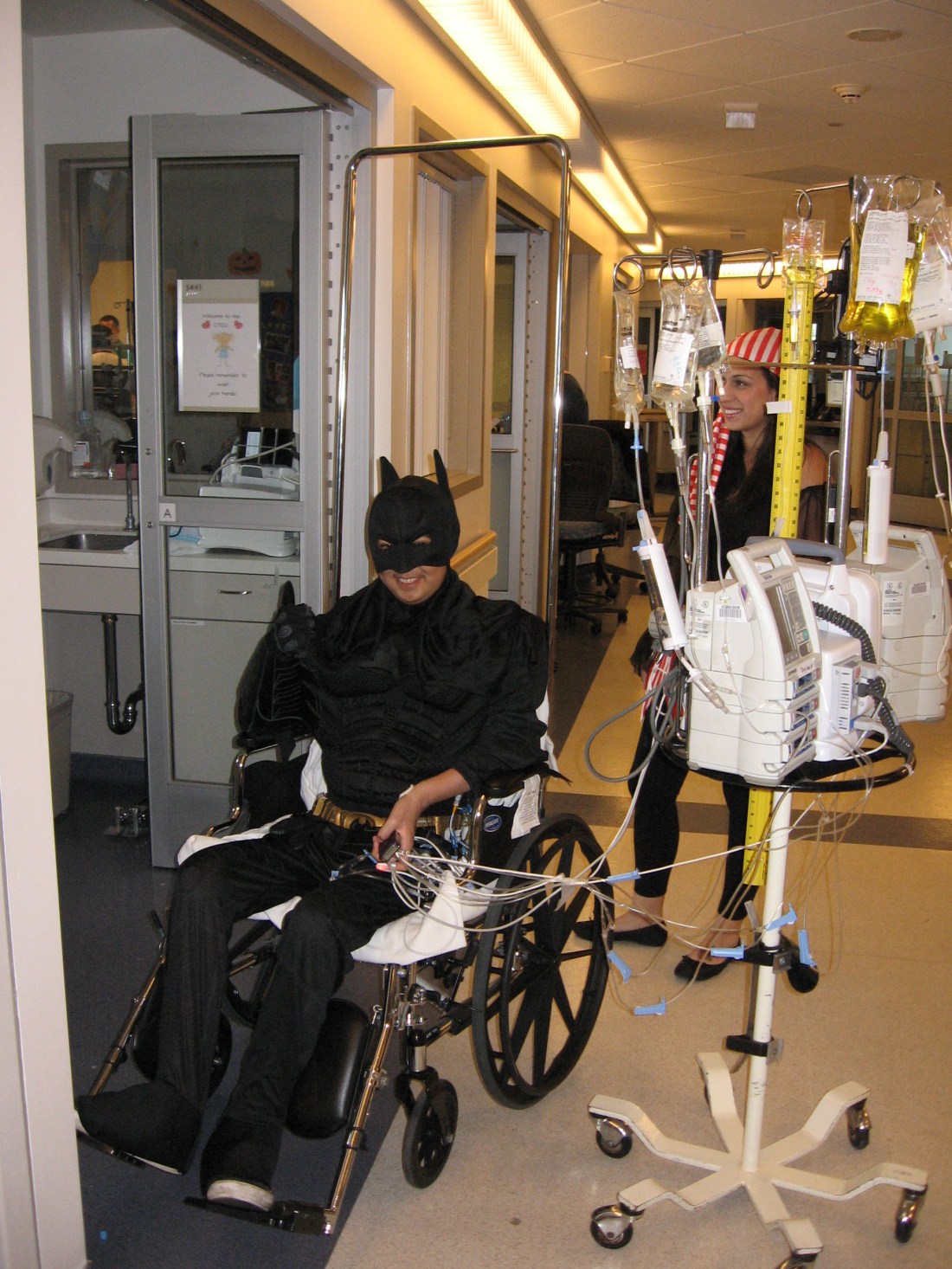
Our formal introduction came on Halloween, when Cesar came rolling down the hallway in his full Batman costume pushed by Liz, his older sister, as he wasn’t going to miss out on the festivities. That evening, I think there were close to a dozen people in his room watching videos and playing video games (Cesar came prepared with his own Playstation). While Rudy wouldn’t know Halloween from any other day, we were missing our kids a great deal that night so there was something comforting in seeing family and friends making sure that our neighbor wasn’t going to miss out on a memorable holiday just because he was in the CTICU. We stopped by as we left sometime after 11pm and were met with expressions that said, “What, you’re leaving already?” Cesar declared that there would be pizza arriving shortly, but since he stopped short of an edict, we begged off and got some sleep.
In the days following, Cesar went for walks about twice a day and always made a point of stopping in. We, in turn, stopped by his room a couple times a day. Through this, we learned that Cesar was also born with Hypoplastic Left Heart Syndrome, went through the Norwood operations and then needed a heart transplant at age 12. He was back in the hospital because he was rejecting this heart and was going to need a second transplant. In learning his kinship with our son, Cesar visited Rudy’s bedside, looked him over and with the authority that comes from experience said, “Rudy’s gonna do really well. I just know it.”
I suppose it’s natural to lament one’s own circumstances, but life in the ICU shows us that there are different flavors of agony and I often walk away from conversations feeling deeply for what people have to face and thanking God for what we’ve been spared. For Cesar and his family, the burden was an angst-laden waiting game. On the one hand, they would have as little as five hours notice before surgery; on the other, the wait could be as long as six months for a donor heart to come available. However long it took, Cesar was going to be in the hospital until a match was found.
In order to survive extended stays in the ICU one is wise to learn from the example of others, so we are so grateful for Cesar and his family. Enrique and Maria amaze us in their ability to extend themselves in maintaining work and family. While Santa Ana is within the LA area, there are likely times where traffic makes the drive about as long as the one from Santa Barbara; yet they are here almost every evening, even if it means driving in late after work for just a couple hours to be with their son. His older sisters, Angie and Liz, are blessed with looks and charm that most likely keep their dance cards full, but they’ve taken an inordinate number of shifts at his bedside keeping him company. While we don’t like for Rudy to be alone here, it seems even more pressing for kids who are more cognizant of their surroundings. So I am amazed at the lengths they go to in making sure Cesar has company.
But most moving is Cesar himself, who goes beyond simply having a positive attitude to embodying a defiant joy. He’s quick with a welcoming wave through the window. Even though his walks down the hallway are slow and require a nurse to push his IV stand and keep an eye on all the lines, my attention is diverted to the huge “Crusty the Clown” slippers on his feet that make the whole scene evoke laughter more than pain. As much as he might drag his feet on some of the assignments he’s had, he’s excited about getting back to school. I’m not sure he has the green light from his parents, but he speaks of getting a Husky puppy when he’s back home and is threatening to name it after one of the doctors.
Make no bones about it, the ICU is a scary place where kids and parents are faced with circumstances that are the stuff of nightmares. To be here is to take up a battle position and wage war against the opponent. We take on any sort of demeanor in such a showdown; we can get angry, hostile, fearful or overconfident as we fight against that which scares us. But leave it to a teenager like Cesar to be the most rebellious. He demonstrates the greatest defiance in laughing before the foe, fully aware of it’s might but unwilling to let it steal his joy.
All hail, Cesar—our conquering hero!

 As exciting as it was to see the ventilator removed and set on “Standby”, it turns out we’re standing by in a larger sense right now. As they got Rudy extubated, Dr. Rick took time for a good listen and did not feel that Rudy was getting enough air to breath with out the machine. Before they re-intubated, they called for an ultrasound which showed that his lungs are functioning as they should but the left diaphragm is not working properly preventing the left lung from getting enough air. We are waiting for further assessment on the ultrasound film.
As exciting as it was to see the ventilator removed and set on “Standby”, it turns out we’re standing by in a larger sense right now. As they got Rudy extubated, Dr. Rick took time for a good listen and did not feel that Rudy was getting enough air to breath with out the machine. Before they re-intubated, they called for an ultrasound which showed that his lungs are functioning as they should but the left diaphragm is not working properly preventing the left lung from getting enough air. We are waiting for further assessment on the ultrasound film.