Busy, busy, busy…training and practice continue as Rudy keeps working on his feeds. His status was upgraded to “floor status” in the ICU which means the nurses check his vitals every few hours instead of every hour and leave most of the treatment care up to me (and Rolf when he comes over the weekend). Yet another step toward home…please pray he doesn’t spike any last minute fevers or develop any last minute infections. Rudy has one more day left on his antibiotics…when he finishes the cycle, they’ll be able to pull his subclavian line (the last line to go) and all other meds will be transitioned to oral doses. I’m praying an infection doesn’t pop up once he is off the antibiotics. He took a bottle for three of his feeds today…the rest were through his g-tube. Right now it takes him about an hour to finish a feeding…the team would like to get it down to 30 minutes ultimately. It’ll take a while for Rudy to learn to eat that quick – it’s an issue of conditioning at this point. So, there will be quite a bit of work to do at home to help Rudy reach many goals…gotta get to work on that “master list” of “to dos”. Old habits die hard!
Month: March 2009
“Good Day, Sunshine”!

Today was a great day…one of the only crisis-free visits we’ve had with Rudy and all the children together. There was no need to usher the kids out of the room because of an “episode”, no frank talks with Drs that left me wiping away tears so the kids wouldn’t see, no family meal in the cafeteria with Rolf and I sitting catatonic…
The kids and I got an early start from home and made it to UCLA at 10am. We found Rudy in Daddy’s lap just hanging out. Max quickly took Dad’s spot and held Rudy for a little bit and then all the children accompanied Dad to his CPR training. Like a good Girl Scout, Olivia was able to answer a number of Nurse Katie’s questions because of her “First Aid” training at a Brownie Troop Meeting this year! I tried to nurse Rudy while they were all out of the room but he wasn’t too interested so I ended up pumping and giving him a bottle. When everyone returned, we packed up the red wagon full of Rudy and his gear and headed to the peds patio…making sure we paraded through the CTICU on our way. It was a beautiful, sunny, breezy day here in L.A. and Rudy’s very first venture outside was a special one with everyone in tow. True to Rudy’s norm, he was asleep for a good big of this momentous occasion but woke up towards the end…

Check out Rudy’s first experience with a little breeze on his face and siblings playing in the background:
Take a look at Rudy’s entourage:
When we returned to Rudy’s room, Rolf and I had a few more “home care” lessons and the kids entertained themselves for a good bit conducting a teddy bear health clinic…



Wilson got his turn to hold Rudy for a bit and before we knew it the afternoon was gone and it was time to drop the kids off at dear friends’ for a couple of days of spring break fun!! Understandably, Rudy was pretty wiped out and had a good nap while we packed up to go. Rolf dropped me off back at the hospital around 9:30pm, said another goodbye to Rudy, and then headed home to Santa Barbara…I’ll stay with Rudy until Wednesday, pick up the kids and we’ll all head home as well to spend the last half of spring break at home – celebrating Wilson’s 12th birthday and making more preparations for Rudy’s homecoming. It was a whirlwind day full of excitement and adrenaline…I think it was quite encouraging for the children to see Rudy doing well and to hear the nurses and docs talk about his discharge. It’s starting to sink in for all of us -Amazing!

Greetings from Camp Wanna-Be-A-Doc!
I’ve had a running joke with the team here that I’m one day hoping to earn a “Junior Doctor” patch. Well, it looks like that’s coming true as Rudy’s room has become kind of like camp. There is a number of things we need to demonstrate competency at before Rudy can go home and, consistent with her temperament, Trish has asked for a list to be compiled which is now posted on the closet door. This weekend Nurse Lindsey is walking us through the day and every time we successfully perform something she notes it on the chart. Sometimes she quizzes us and we even get to practice some things on a very creepy looking doll before we move to Rudy. So far, I’ve received merit badges for trach tie changing, trach suctioning, dispensing meds through the G-tube, G-tube cleaning and securing the pediatrician. Tomorrow morning, I’ll hopefully earn my CPR badge–leave it to me to make this a competition, but I guess I’ve always been motivated by sticker charts.
Since I mentioned her, I just need to say that Nurse Lindsey is the GREATEST NURSE IN THE WORLD! Yeah, she’s highly trained and very skilled at providing acute care for patients who need it. Really grateful for that, but she wins this approbation for stopping at Starbucks on her way in this morning to bring me some coffee. Instead of needing to stumble down into Westwood myself, I got to start my day lounging around in my PJs with Rudy here in the room. Florence Nightingale never did that!

While there’s all this activity to keep me occupied and entertained, Rudy’s impressing us all with the great strides he’s making. We turned off the feeds for an hour twice yesterday and let him try to take the 30cc by bottle–success! Today the team decided to try to compress the feeds to move from constant drips to “bolus” feeds–where it all comes in one shorter burst (as it would in a meal). We were going to proceed incrementally by spreading 90cc over two hours and then to one and try a bit by bottle every now and again, but on the first feed this morning we put 45cc in a bottle which Rudy devoured. So, we filled another bottle and he pretty much gave his vote with regard to proceeding incrementally. It was no fluke–he’s done it twice more, so the order was re-written for Rudy to make the call–he can feed 90cc by bottle every 3 hours, but if he’s sleeping or just doesn’t seem to feel like it, we can put the balance in the G tube. He would appear to have his father’s feeding habits.
On the down side, I’ve re-discovered what I had forgotten over the last six years: all that food going in has to come out in some form and a diaper’s seal far from impenetrable. Full breast-milk feeds have resulted in technicolor emissions that register in multiple dimensions. His brothers will marvel at the sounds and I regret that I only brought one pair of pants with me…
It is a very happy adjustment to be thinking concretely about bringing Rudy home. There’s some open speculation as to what our time frame is at this point, but I suspect we’ll gain some clarity on this on Monday when the new attending comes on. I’ve been reflecting on the post I wrote awhile back on the Stockdale Paradox and how our thinking has undergone a shift. Back in January, we had to hold forth that we would prevail over this circumstance without any real idea of how this would come about. I’m certain I didn’t think we’d be headed into April, but here we are. There were twists and turns enough to turn unrealistic hope into insanity, but here we are. Given that we’ve been here six months, we’re not up in arms if it extends a few weeks more. It’s just such an encouragement to be viewing things through a new lens.
I’m looking forward to a quiet night here with Rudy and hope he rests well for tomorrow when Trish and the kids will be coming for a visit. It’s actually been almost two months since we’ve all been here together. Word has gotten out among the staff that the floorshow will be here in full force tomorrow–can’t wait. These poor ICU people–who will entertain them when we leave?
PS–speaking of fun, Livy made another appearance on the web as Greg Lawler shared everyone’s intrigue about how her trademark “green tooth” dangled precariously without falling out for so long. Good news everyone–it finally “fell” out (with a little help from Daddy during a wrestling session).
A Couple More “Goodbyes”…


I made it home safely this afternoon but before I left UCLA, Rudy and I had a little bottle-time. He continues to do well with the sucking and swallowing but the big adjustment for him is tolerating any volume more than 1 oz at a time in his stomach. Because he is on continual feeds getting 1 oz. a hour, he isn’t used to getting larger volumes all at once. He’ll continue to get bottle feeds intermittently to allow him to practice oral feeds but he will also continue to get feeds through his g-tube. One reason for this is to help conserve Rudy’s energy before his next surgery. Oral feeds require more energy making his heart work harder so, for now, the g-tube will remain.
The jp-tube, however, was removed today! After 24 hours on breastmilk, there continued to be no drainage from the stomach cavity into the tube so we were able to say goodbye to another line and potential source of infection. The next and last line to be removed is Rudy’s sub-clavian picc through which he is getting his meds. Gradually, they’ll transition Rudy’s IV meds to oral meds (or in Rudy’s case, through his g-tube) so they can remove that line before we go home.
Speaking of “goodbyes”, RT J-Way, Nurse Sam and I kissed the vent goodbye late last night! His breathing continues to be strong and steady. PTL!

Rolf will head down tomorrow to spend the weekend with Rudy…the kids and I will join them late Sunday or early Monday. The kids are excited about Rudy’s progress and all our talk of bringing him home. We’re all excited but also not quite believing it’s true!!! It’s all a little hard to comprehend.
Got Milk?
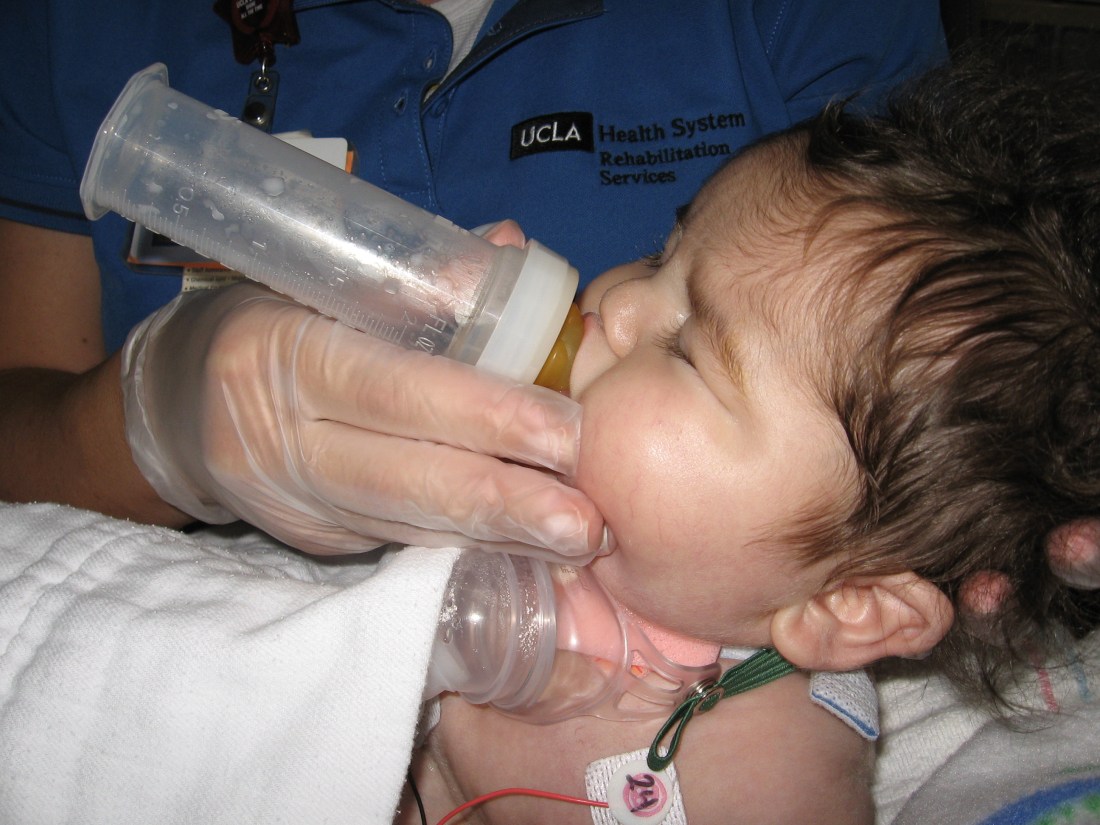
Check out our super star today…he took to a bottle of breastmilk with great ease and showed-off for OT Nicole how he can down 15ccs (=1/2 ounce) in 2 minutes!! Ha Ha Rudy reached the goal of full feeds (30ccs/hr) around 3am…they started him on breastmilk this morning at 11:00am and as of 9:00pm there hasn’t been any fluid drainage…they’ll want to watch it close for 24 hours but so far so good! Today is also Rudy’s first full 24 hours on the trach collar and he’ll stay off the vent indefinitely at this point. I think it’s kind of interesting that he reached both target goals on the same day! Break out those beads!!!
As for me, well, my day was rather full. I was trained in CPR for an infant with a trach and in the daily trach cleaning process as well as the cleaning of the g-tube AND I changed out Rudy’s trach for the first time (something we’ll have to do at home once a week). It all went smoothly. All of Rudy’s care will be time consuming, at first, but doable. My biggest concern in bringing him home, at this point, is keeping him infection-free between now and his Glenn surgery…don’t be surprised if you see our family walking around with travel-size bottles of hand sanitizer hanging from our necks! 🙂 Rudy’s room was one continuous string of folks coming in to talk to me about all kinds of treatment details. We’ve only just begun this discharge process and already there is too much information to process and retain but like we’ve done from the very start of this journey we just need to take it ONE DAY AT A TIME.
Rudy and I got to say our first “goodbye” today to Dr. Rick. He will be gone the next two weeks and he came in to say goodbye at the end of the day because, as he said, he hopes we’ll be gone when he gets back. Ha Of course, we’ll see him soon enough at our follow-up appointments for which we’ll need to come back but it was nice to say an official goodbye nonetheless…another step closer to home.
Speaking of home, I hope to get an early start for SB tomorrow as I’d like to stop at WalMart on the way to get a crib mattress and sheet for the little lad. Rolf will come for his normal weekend shift with Rudy and then the kids and I will come to LA for a couple of days early next week for the start of their spring break. We might get to take Rudy outside for the first time (on the peds patio on our floor) on Monday if I can get it coordinated with the nursing staff and folks over at Child Life. Please pray the logistics of that outing will come together…it sure would be a special moment to share together as a family. The first of many, many shared moments to come, we pray!! Lovin’ you all from Rudy’s room…
Time for Milk!
Trish just called with an update so I’m putting up a quick post. Rudy has been at full feeds (30cc) since 3am and everything continues to go well. So, in the next hour they are going to switch him over to breast milk. We know now that his stomache can process at the volume it needs to, now we need to know if it can process fats without there being any chylous fluid coming out of his lymph system. The JP drain is still in, but probably won’t last much longer, so the plan is to start milk in the next hour and see what comes out of the drain–please pray for NOTHING!
Happy 25-Week Birthday
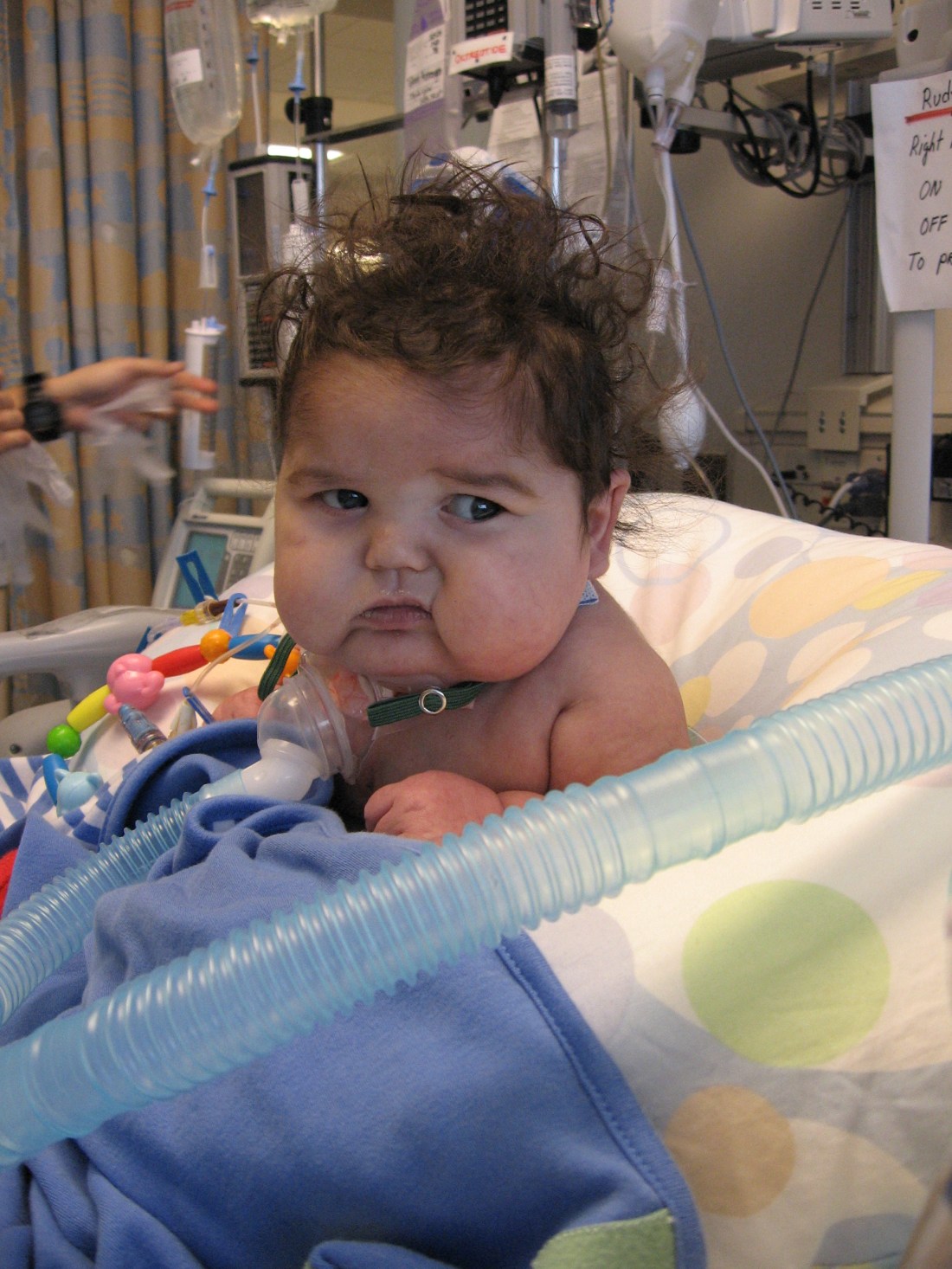
Hooray! Hooray! The little superstar passed his swallow test!! It was really quite remarkable to watch the images on the flouroscope…you could tell right away that the contrast fluid was going down the way it’s supposed to. Speech therapist Carol conducted the test and gave Rudy the contrast through a syringe at first, halfway through the test she said, “He’s really sucking on this syringe, I’m going to try a bottle”. The minute she gave him the bottle, he latched onto it like a pro and drank from it with no problem. The whole thing brought me to tears. OT Nichole came down to watch as well and we gave each other a big hug in celebration of Rudy clearing yet another really big hurdle. Like I told Dr. Rick when we returned from radiology, it’s just so nice to have a definitive, no-doubt-about-it, POSITIVE result where Rudy is concerned! Everyone who heard the news was quite excited for Rudy and his BIG step toward home.
There was alot of talk about discharge details today so that certainly added to the excitement. We’re still a couple of weeks away from bringing Rudy home (at least) but it is helpful to get started on the many details that need to be addressed. I go to CPR class tomorrow morning and get trained to do CPR on babies with a trach. Rolf and I both need to practice suctioning Rudy’s trach and learn how to change the trach completely as that will need to be done each week. We’ll need to learn how to care for and administer feeds through his g-tube, etc. We need to find Rudy doctors up in SB and start getting things settled for him at home. Wow, there are so many things to think about right now!!
I tried to put aside the rush of details in my head this afternoon and focus on a little sucking therapy for Rudy. He is clear to start the non-nutritive sucking therapy so we tried it for the first time. I brought him to the breast after pumping empty (he’s not allowed to ingest the breastmilk yet) and let him “find his way”. It’s definitely a new feeling for him and I’m not too sure what he thought of the whole thing but he did finally relax and got comfortable sucking. He isn’t quite latching on securely but he’ll get there…it’ll take some practice and I think he’ll be more motivated to latch on when he’s allowed to drink the milk while nursing. So fun and crazy!!! One of the charge nurses said she has never seen a baby as sick or as intubated as long as Rudy do so well at the swallow test or take so quickly to nursing…our prayers are being answered.
So, the process continues forward…Rudy is currently at 28ccs/hr on his feeds through the g-tube. They’ll, most likely, introduce breastmilk tomorrow and it could take a couple of days to see if the chylous fluid will return. If it does return, he’ll go back on the Tolerex formula and I’ll look more closely at what it will take to skim my milk of it’s fat. If it doesn’t return, then we can get rid of the Tolerex finally start using the MEGA-supply of mama’s milk we have stashed away in the unit! Rudy will spend a total of 22 hours off the vent today which means they will bump it up to 24 hours tomorrow!!! At that point, he’ll stay off the vent and they’ll monitor him closely for a couple of days before declaring him “vent free”. Other than that, he has a couple of meds they need to start weaning him off of and the surgical team will remove his “frankenstien stitches” early next week. Things are falling into place…finally!
We’ll never know what tomorrow is going to bring but it sure is wonderful to end a day with Rudy with a strong sense of hope for a brighter tomorrow.
No Big Gulps Today!
I don’t have much to report this evening as the swallow test was rescheduled for tomorrow at 11am. ‘A little disappointing only because I’ve been waiting soooo long to get going on this non-nutritive therapy but it’s not a big deal to wait another day. What this means, though, is that they are going to keep Rudy at his current setting of 27 ccs/hr, they’ll have to stop his feeds tomorrow morning before the swallow test, and then we’ll pick up on the feeds at 27ccs/hr again after the test…we may not get to 30ccs tomorrow afterall but, again, hopefully it will be a short wait. 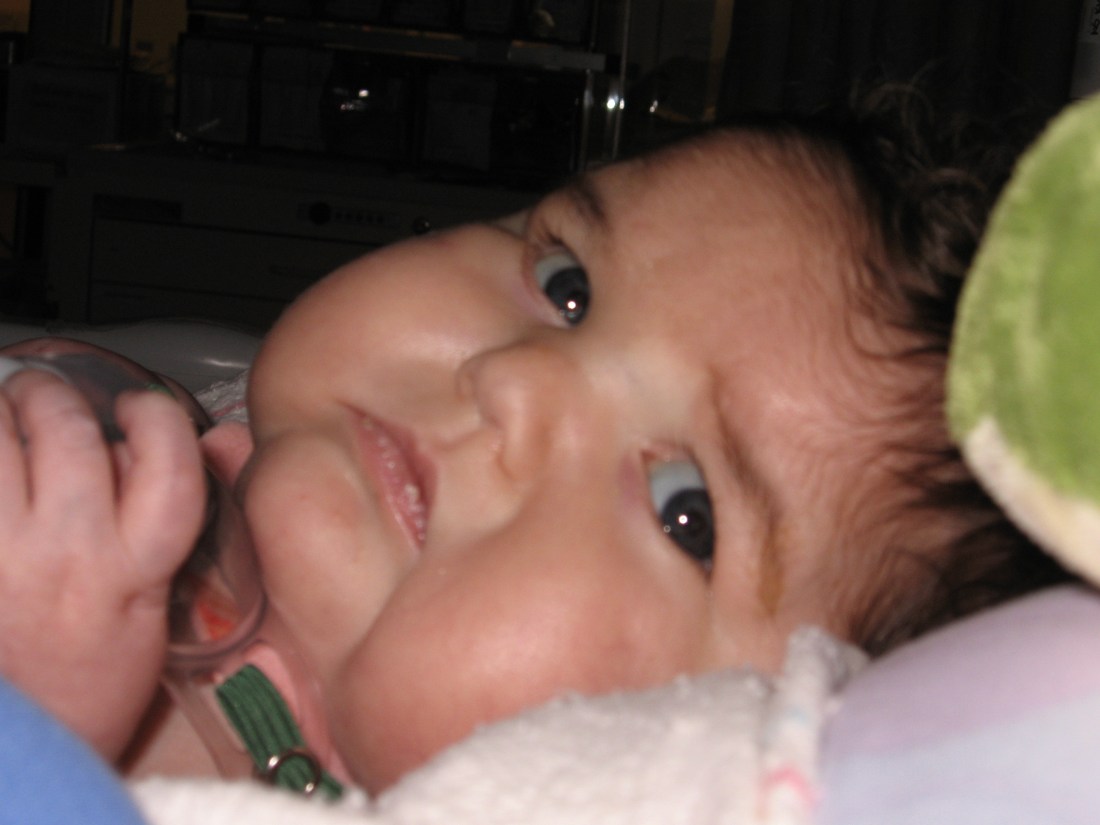
Other than the disappointment of the short delay on the swallow test, today was uneventful. RT Oscar was assigned Rudy today which was fun as we hadn’t seen him in a few weeks. Nurse Sandy made me laugh out loud when she came back after lunch sporting a gorgeous 3 diamond ring a little freaked-out…it belonged to another nurse friend of hers and Sandy tried it on for fun while they ate lunch together. Her friend suddenly got paged to go down to the OR and left in a hurry WITHOUT her ring!!! Nurse Sandy was so nervous she was going to lose her friends ring she ended up taping it to her finger…what a hoot!!!! The ring was returned at the end of the shift and Sandy was definitely relieved!! 🙂


Progress Continues…
Sorry for the delay in getting an update out…’hope it wasn’t cause for worry to our faithful “Beat” readers! 🙂 I ended up holding Rudy last night after a late dinner until 1:30am so my usual evening post got sidelined. I’ll be sure to post a longer update later this evening but, for now, I’m encouraged to report that Rudy continues to move forward!
He did great with his 18 hour trach collar sprint yesterday so the order for today is 20 hours…Nurse Practitioner Anita said yesterday that once he is weaned off the ventilator they’ll want to watch him for a few days (possibly a week) before sending him home – we’re getting very close to that 24 hour goal so the next several days will be key in terms of determining whether or not he’s ready to be off the vent completely…you may recall that he made it 5 days off the vent before but he definitely looks like a different baby this time around…not labored in his breathing at all. We’re encouraged.
His feeds are going well too! Rudy is now up to 26ccs/hr and our goal is to get him to 30ccs by tomorrow afternoon. Once he hits 30ccs/hr, then we will introduce my breastmilk again. If he tolerates the full-strength breastmilk and there is no drainage output, then the drainage tube will be removed sometime this week. Please pray for this specifically…that Rudy’s body will respond well to breastmilk and soak it up like a sponge!!! This, too, will be a key turning point for Rudy. We’re scheduled to take a trip to Radiology (hopefully sometime today) for a swallow test. We need the test done before Rudy and I can begin non-nutritive suckling therapy…it’s something OT helps us with initially and then I can do it with the help of our nurses but it’s basically a process where I pump myself empty and introduce him to the breast. He’s not ready to take in milk orally yet but if we can teach him how to latch on now then he’ll be ready to go when the time comes…again, though, this all depends on wheather or not his body will absorb breastmilk so there is alot emotionally riding on the next couple of days for me.
So, hang tight…I’ll let you what comes of this swallow test later today! Big hugs from Rudy’s room…
Homage to a Hero: Dr. Rick Harrison
From Rudy’s new room, I can look across the nurses’ station to his old one and it brings back memories of those first days when this whole place was so unfamiliar. I remember being overwhelmed by mysterious pieces of equipment being wheeled around. I remember trying to divine the purpose of many procedures I had never seen before. I remember the parade of people coming in, introducing themselves, their specialty and then examining Rudy. The raw intensity was such that most of the names escaped me well before their bearer even left the room.
A few repeated faces started to distinguish themselves amidst the blur of those first few days. Rudy’s condition was very tenuous at that point and there was lots of attention being paid to him and all the foreign numbers up on the monitors. The doctor with lively ties seemed to be in the room quite a bit, watching carefully. Like everyone else, he watched the numbers tick by, but gave equal amounts of time to watching Rudy—noting his skin tone, the flare of his nostrils and the cadence with which his chest would rise and fall. Even when he was dealing with other kids in the unit, most of his passes by the room included a quick scan and status check.
It was only the most disciplined restraint that kept us from constantly cornering every doctor for detailed explanations on what they were doing and seeing. There was an instinctive sense that hovering over the staff would interrupt their work and divert the attention that needed to be paid to Rudy. But even if he couldn’t give a running commentary, the doctor with the ties always seemed to stop at just the right time to give us an update on what was going on.
Dr. Henderson? Dr. Haroldson? Doctor Richardson? For some reason it took me quite a few quiet checks with nurses to get straight on the name, but finally I got it that the Doctor with the ties was Rick Harrison. Remembering his name at this point isn’t much of a challenge as Rick is the second intensivist who has done the bulk of the rotations during Rudy’s sojourn here in the ICU.
I’m not sure how one could navigate such a journey as the one we’ve been on without trust in the people we simply need in order for Rudy to have a chance. As I’m continually impressed by the giftedness and knowledge of most every nurse, tech and therapist, I have nothing but awe left for the doctors. In position, but more importantly in competency, Rick is at the top as he brings incredible expertise and clinical experience into the very emotional arena of very sick children and the fretful parents that accompany them.
As much as I’d love to cling to the notion that no one knows my child better than I do, I probably let go of it well before Rudy was born. No one loves him more, but it only takes one visit in rounds to be reminded that there are levels of detail I’ll never understand and questions I wouldn’t even think to ask. For Rudy’s sake, I’m grateful there is expertise that far surpasses our own. I’ve come to see that his treatment rarely involves black-and-white decisions; but an involved sequence of judgment calls requiring knowledgeable coordination of disparate and often intricate steps. We are grateful for the many weeks that Rick, with his measured and seasoned expertise, has played this central position.
A good doctor at this level is deeply knowledgeable, drawing on science and experiences with thousands of patients. An exceptional one also recognizes that each patient is unique and at some point departs from the textbook conventions. We have often heard Rick remind the doctors in rounds that Rudy has his own norms. He is probably more intricately aware of the data than anyone else and would never flippantly dismiss it, but his overall assessment leaves room for common sense and basic observation. As helpful as science is, a skilled clinician knows when it should be trumped by simply looking at whether the patient looks peaceful or distressed.
We never lose sight of the fact that Rudy’s condition has us in a place of dependence and we are so grateful that one of the key people we are leaning on is one we trust so deeply. Trish and I have daily discussions about Rudy’s course of treatment, and more often than not they touch on Rick’s opinion. Rick’s esteem among his colleagues seems to match ours as I can’t recall anyone being offended by the many times we’ve asked if he’s been consulted. It was only in gathering my thoughts to write this that I discovered that Rick wears another hat—as Medical Director for the Mattel Children’s Hospital. As far as we can see, they sure have the right guy in charge.
We place our trust in Rick not only because of his technical competency, but also because of his ability to appropriately straddle clinical distance. This journey is about my kid and I’m a human being going through emotions that I’ve never experienced before as I try to comprehend realities I never dreamed I’d have to face. So, I need guidance from human beings, who never lose sight of the seriousness of the situation or some form of necessary objectivity; but don’t engage without emotion. They hurt with us; are frustrated with us; know the process well enough to identify milestones worth celebrating; and introduce well-timed humor amidst circumstances so intense it would never be expected. In light of this, my most vivid memories of Rick do not center around medical details, but on human interactions: celebrating when Rudy peed enough; overseeing Rudy’s first two extubations; losing more than a couple nights’ sleep at home pondering Rudy’s condition; feeling sad and frustrated with us when we had to go the route of the tracheostomy and feeding tube; and stopping in on an off day to see Rudy and Trish after hearing of the chylous fluid in Rudy’s stomach.
Rick describes himself as “the doctor no one wants to see”; because dealing with him means you have a very sick child. Point taken, but given that I have no choice over the condition Rudy was born with, I can’t tell you how glad for the many times we have seen Rick.
